Tag: heidmann
When dressage rider Meagan Davis and owner Scott Durkin think about the goals they have for their dressage horse Royale, they have tunnel vision for the grand prix ring. Royale, a 16-year-old Oldenburg gelding (Routinier x Ironman) was well on his way to accomplishing that goal during the 2019 season when something strange started happening.

Photo courtesy of Meagan Davis
After arriving at their winter home in Loxahatchee, FL, from a northern base in Stone Ridge, NY, Davis kicked off Royale’s winter competition schedule with a show in January. The horse was coming off a very successful fall season that included CDI Intermediaire I and CDI Prix St. Georges victories at the New England Dressage Fall Festival and Dressage at Devon.
“Our first show was unusually chilly and I noticed that Royale was breathing a little hard and didn’t sweat very much,” recalled Davis. “I didn’t think that much of it because of the weather, but when we returned home and it warmed up, he wasn’t sweating at all.
“He could not catch his breath after being perfectly fit a month before,” continued Davis. “I rely on Palm Beach Equine Clinic for the care of all the horses in my barn and I immediately turned to Dr. Robert Brusie.”
Dr. Brusie is a Board-Certified Surgeon at Palm Beach Equine Clinic and was diligent about ruling out any physical causes of Royale’s obvious discomfort and decline in performance. After flexion tests, checking for musculoskeletal problems, and assessing soreness or wear and tear, Dr. Brusie turned to Palm Beach Equine Clinic’s Internal Medicine Specialist Dr. Peter Heidmann.
“Dr. Brusie was watching me work him one day, noticed the decline in muscle, the lack of sweating, and labored breathing, and recommended we take a deeper look with a specialist,” said Davis. “That is why I trust Palm Beach Equine Clinic with the care of my horses. They have so many tricks up their sleeves, and their clients are fortunate that the veterinarians collaborate so well together in order to do what’s best for the horse.”
Dr. Heidmann’s first step was to asses any neurological causes by testing for equine protozoal myeloencephalitis (EPM) and Lyme disease. Both were negative. He then moved on to a nutrient analysis.
“When you see weakness and poor muscle mass in a horse, two of the things you test for right away are vitamin E and selenium deficiencies,” said Dr. Heidmann. “Both are common causes of decreased performance due to low concentrations in local soil or the soil where a horse’s hay derives from.”
No deficiencies were found in Royale, which prompted Dr. Heidmann to move on to muscle testing. He drew blood from Royale, put him in work, and then drew blood again four to six hours later. When comparing enzymes in the blood from before and after work, Dr. Heidmann looked for any large increase, which would indicate the problem was in the muscles themselves. Royale’s tests, once again, came back normal.
At this point, Dr. Heidmann returned to the case history and started following the shortness of breath symptom, noting, “Breathing abnormalities in horses are difficult to diagnose by simply listening because their chest wall is so thick. What I wanted to asses was prolonged recovery. This is done by placing a bag over a horse’s nose to get them to breathe deeply. Once the bag is removed, breathing should regulate within two to three breaths. Royale needed four to five breaths.”
Once Dr. Heidmann identified a possible cause, he performed abronchoalveolar lavage (BAL), which is essentially a lung sample used to identify abnormal cells. He inserted a small-diameter tube through the trachea, flushed saline into the lung, and then suctioned it back out.

“Sure enough, when I examined the sample, there was mucus and abnormal cells,” said Dr. Heidmann. “Despite his bloodwork being normal and no obvious infections, Royale was battling equine asthma or ‘heaves.’”
The treatment for asthma in horses is very similar to what’s done for humans and includes an anti-inflammatory bronchodilator drug and inhaled steroids.
“While his breathing issues were significant enough to affect performance, Royale’s treatments were relatively mild with immediate and substantial improvement,” said Dr. Heidmann. “I used nebulized herbal remedies, steam, and Ventipulmin, which is an oral syrup.
“I’m a less-is-more person and veterinarian,” he continued. “I try to have the best outcome with the least amount of medications. Additionally, we created some routines that would minimize environmental dust and allergens, such as using a hay net, wetting down hay and bedding, or using chopped newspaper as bedding.”
Royale stayed on the prescribed medication through his trip home to New York and came off them at the end of May. Today, he is back in work and has regained the fitness and muscle he had during the fall. According to Davis, their goal is to step into the grand prix ranks during the upcoming season.
“My favorite cases are the sickest of the sick and the most elusive needle in a haystack,” concluded Dr. Heidmann. “Royale’s case definitely fell into the latter. It was really challenging, but rewarding because the outcome was a horse that is dramatically different than he was four months ago. But the most important part of this case for me was working together with Dr. Brusie. I would have not been successful in helping this horse if he hadn’t done all the work prior to coming to me. That kind of collaboration is what contributes to our success and sets Palm Beach Equine Clinic apart!”
Internal Medicine: What’s it all about?
Palm Beach Equine Clinic President Dr. Scott Swerdlin often says, “If you want to attract equine veterinary specialists, you have to have impressive facilities and technology in place.” Palm Beach Equine Clinic is one of the few veterinary clinics in the country to offer clients the talents of board-certified specialists in nearly every branch of equine veterinary medicine. One such specialist is Peter Heidmann, DVM, DACVIM, a graduate of Tufts University School of Veterinary Medicine, who joined Palm Beach Equine Clinic in 2016.
Dr. Heidmann specializes in the treatment of internal medicine cases at Palm Beach Equine Clinic.
What attracted him? The facilities! In the heart of South Florida’s horse country and at the center of the busiest winter competition schedule in the world, Palm Beach Equine Clinic boasts an internal medicine and infectious disease center at its Wellington-based clinic.
The crown jewel of the center is the ability to stop airborne disease dead in its tracks with the U.S. Department of Agriculture (USDA) approved isolation stalls that completely enclose horses in their own environment with individual filtered airflow systems that do not reach other horses. On top of secure isolation and individual airflow systems in their internal medicine facilities, Palm Beach Equine Clinic also constructed areas for each stall where medications are prepared, equipment is stored, and dirty bedding is handled.
To further mitigate risk, veterinarians, technicians, and staff take every available precaution, including foot baths before entering the stalls and wearing personal protective equipment such as Tyvek suits, gowns, and face masks to provide multiple layers of protection against spreading disease. In some cases, a specific team of doctor, technician, and intern is assigned to a patient and won’t touch another horse for the duration of the treatment.
Accurately Diagnosing Internal Medicine Cases
Diagnostics is not a guessing game at Palm Beach Equine Clinic. With advanced imaging equipment, including a computed tomography (CT) machine, standing magnetic resonance imaging (MRI), and nuclear scintigraphy camera (bone scan), as well as radiography (x-ray) and ultrasonography capabilities, Palm Beach Equine Clinic is armed and ready to quickly and accurately diagnose internal medicine cases.
Dr. Heidmann refers to the facilities and his work at Palm Beach Equine Clinic as a luxury, saying, “I’ve managed many cases in various facilities going all the way back through internship, fellowship, and residency, but this is as nice as any place I have ever worked. It makes the risk to the horses so much lower, but also removes the anxiety for myself because I’m able to look a client in the eye and tell them that there is no risk. I don’t have a concern about disease spreading from one patient to another because at Palm Beach Equine Clinic we have the tools that we need.”
Understanding Internal Medicine
To understand how diagnostic tools are most effective, one must understand what exactly internal medicine is. In an effort to define internal medicine, Dr. Heidmann noted, “What you’ll see on the American College of Veterinary Internal Medicine (ACVIM) website is an emphasis on organ systems and organ system problems – respiratory disease, gastrointestinal disease, and neurologic disease being three of the most prevalent.
“What it really entails is a way of analyzing problems specific to the organ systems,” he continued. “It can be all over the map, and that’s part of what makes the specialty so fun and interesting.”
The most common internal medicine cases can be split into three categories:
- gastrointestinal (GI) problems
- neurological system issues
- respiratory diseases.
Gastro-Intestinal Problems in Horses
“When it comes to GI issues, I usually see horses in two categories,” said Dr. Heidmann. “Number one are the horses that may need to go to colic surgery and the horses that just had colic surgery. The other is horses with intestinal infections, often colitis in which they have heavy diarrhea.”
According to Dr. Heidmann, all of the treatments for colitis tend to boil down to the same thing: replacing their ongoing losses and letting the intestine heal itself. It doesn’t matter if it’s colostrum, salmonella, Potomac Horse Fever, or any other kind of infection.
Equine Neurologic System
The nervous system in a horse is made up of the brain, spinal cord, and several different kinds of nerves that are found throughout the body. These create complex circuits through which animals experience and respond to sensations. Unfortunately, many different types of diseases can affect the nervous system, including birth defects, infections, inflammatory conditions, poisoning, metabolic disorders, nutritional disorders, injuries, degenerative diseases, or cancer.
“Palm Beach Equine Clinic has an incredible ability to do advanced imaging and diagnostics on neurologic conditions,” said Dr. Heidmann. “With equipment like the standing CT, we can do scans of the head and neck with contrast – a CT myelogram – which really increases our ability to diagnosis a condition.”
Palm Beach Equine Clinic is able to locate problems not only on the top or bottom of a horse’s neck, but also on the sides of the neck – an area previously inaccessible to view even from myelograms under anesthesia.
“That’s part of the satisfaction of the job that I do; It’s not just ‘here is my experience and here is what I guess is going on.’ I have all of these options at my fingertips for diagnostics and tests. We can confidently confirm our clinical suspicions and then do treatment based on that.”
Respiratory Disease in Horses
As common as a cold for a human or acute in nature, Dr. Heidmann further breaks down the different kinds of common respiratory disease in horses into three categories:

One of the repeatedly praised and recognized characteristics of Palm Beach Equine Clinic is the great pool of talented professionals from all specialties that make up the large team. In 2016, Dr. Peter Heidmann, DVM, MPH, began working with Palm Beach Equine Clinic for the winter season, and this year, the accomplished internal medicine specialist is returning to work with Palm Beach Equine Clinic for the duration of the 2018 winter season.
Dr. Heidmann graduated from Tufts University with his veterinary degree in 2000 before beginning a one-year internship in equine medicine and surgery at Arizona Equine, followed by a one-year surgical fellowship at Oregon State University, followed by a residency for internal medicine at the University of California, Davis, which he completed from 2002 to 2005. In 2005, Dr. Heidmann joined a private equine practice in Montana, and today he is the owner and hospital director of Montana Equine.
Q: What prompted you to pursue equine veterinary medicine?
I knew I wanted to be a vet for a long time, but I didn’t know that I wanted to practice more individually focused medicine until I was going through vet school. It wasn’t until my fourth year, where you’re actually starting to work with patients, that I made that realization. I started moving in that direction, and I had some faculty that saw the same for me and encouraged me to do the horse stuff. I always loved working with horses, but up until that time, I thought my background was too agricultural to do high-end sport horse work. But their encouragement helped me realize that wasn’t true. Then, I decided as a result of that realization and thought process, that I wanted to do an internship and residency to become specialized in internal medicine.
Q: What led you to Montana, and how has your role and practice evolved from when you started there in 2015 to today where you’re now the owner and hospital director of Montana Equine?
When I finished my residency at Davis in 2005, I wanted to be in the west. I wanted to be somewhere where there was nobody with my skill set – meaning internal medicine. I wanted to be in a small mountain town basically. Somewhere that I could practice the kind of medicine that I was trained to do but not in big metropolis. So, I narrowed it down to a practice in New Mexico and a practice in Montana. I went to work for a practice in Bozeman, MT, in July of 2005 and six months later my predecessor, Dr. Dave Catlin, passed away in a car crash. It was really sad. He had three kids, left a widow, and it was his dream to start an equine only specialty vet hospital, which he had done in 1999.
When he died, the conventional wisdom around Bozeman was, ‘Well this can’t be done. Dave had a dream, and it’s not a realizable dream now. There aren’t enough people here. Montana residents won’t understand specialized medicine and they won’t pay for it.’ I was faced with this proposition of leaving the practice after just arriving there, but I knew that was where I really wanted to be. I basically picked up the pieces of Dr. Catlin’s practice and formed Montana Equine in February of 2006.
Now we have a 7,500 square foot hospital with a surgery site at Bozeman, and I have a partner there, an associate, and two interns. We have two satellite locations: an ambulatory-only satellite in Helena, MT, and have nearly completed satellite clinic building in Billings, MT, which is the largest community in Montana.

Q: You began working with Palm Beach Equine Clinic during the 2016 Winter Equestrian Festival (WEF) season, but you’re out in Montana and have your own practice there. How did that relationship come about, and what does it look like today?
There are various aspects to that. We’re very quiet in Montana from basically Thanksgiving through March, and it’s not really my personality to sit around. That’s one aspect, and another is from a business perspective, it allows me to bring more vets on and keep them year-round. A third element is the desire to do more high-end medicine, and a fourth element that led me to Wellington, is my wife, Allison, who is a professional jumper rider. Two years ago, during the winter of 2015, Allison had a girlfriend who had just had a baby and asked Allison to run her business for her here at WEF. I thought that was an interesting idea and started talking to Palm Beach Equine Clinic and found that there might be a need for an internal medicine specialist in their group. So that’s when I started coming. At that point, I was in Wellington for four or five days and then home for ten days, back and forth and back and forth. Then last year, I was more of a week here and a week at home. We had our first child, so Allison and Oliver, who was brand new then, were here straight through, but I went back home to Montana as well. The need is there and the relationship is great. So, this year, I’m in Wellington full-time for the WEF.
Q: What do you enjoy most about having the opportunity to practice with Palm Beach Equine Clinic?
It’s a huge group of people, so there are a lot of personalities. When you have a lot of different personalities, you have a lot of different perspectives on treatments, and that’s interesting and fun. It means that every year when I’m here, it’s pretty dynamic. Back in Bozeman, I have a great team, but I’m the leader of the team. I’m the oldest and the most experienced. That’s good, and that’s not to say that those guys don’t definitely come with new ideas, but being here, there are so many ways of doing things that I end up picking up new tricks or new ideas even though I’ve been practicing for most of two decades. So here at Palm Beach Equine Clinic, I’m picking up new strategies and new techniques separate from new stuff coming out in the world – just different ways of doing things, and different experienced veterinarians to bounce ideas off of. That’s really refreshing and stimulating.
From a vet’s perspective, with the Wellington demographic there is sometimes less of a limitation on budget and expense, so we’re really able to set that factor and worry aside and instead focus solely on what is best for the patient. The limitation isn’t financial; the limitation is just medicine and what we are able to do, which is exciting and allows us to see great results.
Q: Have you had any favorite cases or standout moments during your time with Palm Beach Equine Clinic thus far?
I won’t name any in particular, but what I really enjoy are the challenging medical cases, the internal medicine cases that tend to be really sick and that you’re able to fix. The most common ones that we see are probably sickness after colic surgery, horses with really bad diarrhea, so colitis cases, followed by foals. Those cases generally all have a lot of things going on in a lot of different organ systems. So, there are a lot of factors to balance. Internal medicine people like me are kind of inherently nerdy, and we really get into what’s happening with the acid-base status, electrolytes, blood gases, fluid volumes, and other technical aspects of horse medicine.
Q: What do you enjoy doing outside of work?
While in South Florida, we’re basically working all the time, so not as much here except trying to get exercise and be fit. I like to ride a bike or go for a run. At home, the Gallatin Valley – which is where Bozeman is – is surrounded all around by mountains. The valley floor at Bozeman is at about 5,000 feet, and the peaks are at 8,500, so you can do a lot of really serious hiking. Our son is only 18 months old, but he loves it. I’ve had dogs in the past where their whole personality changes when you get out of town, and that’s what Oliver is like too. It’s almost like his whole face is a different face when he’s out there.
Diarrhea can be a common problem for horse owners, but how do we know when it is serious? What are some of the causes? How do we treat severe cases and what potential complications you should watch for? Internal Medicine Specialist Dr. Peter Heidmann of Palm Beach Equine Clinic in Wellington, FL, has the answers to these questions and more.
Diarrhea, defined as loose stools, or excessive and overly-frequent defecation, occurs when the intestine does not complete absorption of electrolytes and water. Simple changes in feed, exposure to lush grass, or a bite of moldy hay can cause brief irritation of the bowel, giving a horse diarrhea for a day or two, but anything more than that could be from a variety of more serious causes. Bacteria, viruses, and toxins are all factors that can damage the lining of the bowel and lead to equine diarrhea and other complications.
Causes of Equine Diarrhea
The organisms that cause equine diarrhea are mostly bacteria –Salmonella and Clostridium difficile are among the most common. Clostridium difficile is associated with antibiotic use in both people and horses. While antibiotics are useful to kill bad bacteria, they can also kill good bacteria at the same time, upsetting the balance of flora in the body. If a horse goes on antibiotics for any reason, such as a wound or an infection, that can upset the good bacteria in the intestines and cause bad bacteria, such as Clostridium difficile, to grow.
Clostridium difficile can be found naturally in the environment. There are various types of Salmonella, most adapted to birds or to cattle or other livestock, so horses that are around livestock have a higher rate of becoming infected with that particular bacteria. Horses can also carry Salmonella and not have any symptoms, so they can pass it to each other. If the healthy flora in the horse’s body is thrown off by even a small change in diet, or something bigger like a colic episode, or antibiotics, then Salmonella can grow up in its place.
Another bacterial cause of equine diarrhea can be a disease called Potomac Horse Fever. A bacteria called Neorickettsia risticii, which is carried by snails and conveyed by flies like caddis flies, causes Potomac Horse Fever. For this reason, horses that live near rivers or streams can become infected. During warm weather months, caddis flies pick up the bacteria from the streams and can transfer the disease to nearby horses that accidentally eat the flies or larvae. There are hotbeds for Potomac Horse Fever throughout the U.S., including the Potomac basin where it was first described, as well as many parts of the East Coast, and areas of Oregon, northern California, and Montana.
A viral cause of equine diarrhea commonly seen is Coronavirus. This gastrointestinal virus shreds the intestinal lining and can cause horses to become very sick. The body has to reline the bowel, and it does so quickly, but it takes three to five days, during which the horse may have severe diarrhea and secondary infections.
“Coronavirus was thought for a long time to just be an opportunistic infection and that the virus would take advantage of the horse already being sick, but now it is more and more believed to be the cause of its own type of disease,” Dr. Heidmann stated. “Like all of these diseases, it causes damage to the lining of the bowel and supportive care must be used to help the horse heal. Unlike bacterial infections, however, you cannot directly treat the organism, since there aren’t appropriate drugs to directly treat coronavirus in horses.”
Outside of the infectious causes of equine diarrhea, there are mechanical causes, such as ingestion of sand, which can be a common problem in locations like South Florida. Sand is irritating to the lining of the bowel and can cause damage from its weight, as well as its abrasiveness. In general, sand is irritating enough that the body cannot retain the fluid that it needs in the intestines. As a result, it will cause secretory diarrhea where too much water is being lost. Clearing the sand usually solves the problem and the bowel is then able to reestablish a healthy lining.
A final cause of diarrhea in horses is toxins. Toxic plants, such as Oleander, can be fatal in large doses, but if ingested in small amounts, can be a severe irritant to the bowel. Other toxins that a horse can ingest in the environment, such as phosphate or insecticides, may also cause diarrhea.
Treatment for Equine Diarrhea
The single most important treatment for diarrhea, no matter the cause, is supportive care. Supportive care includes providing intravenous fluids to replace the fluids lost, providing protein in the form of plasma for the protein lost due to lack of absorption, as well as balancing electrolytes.
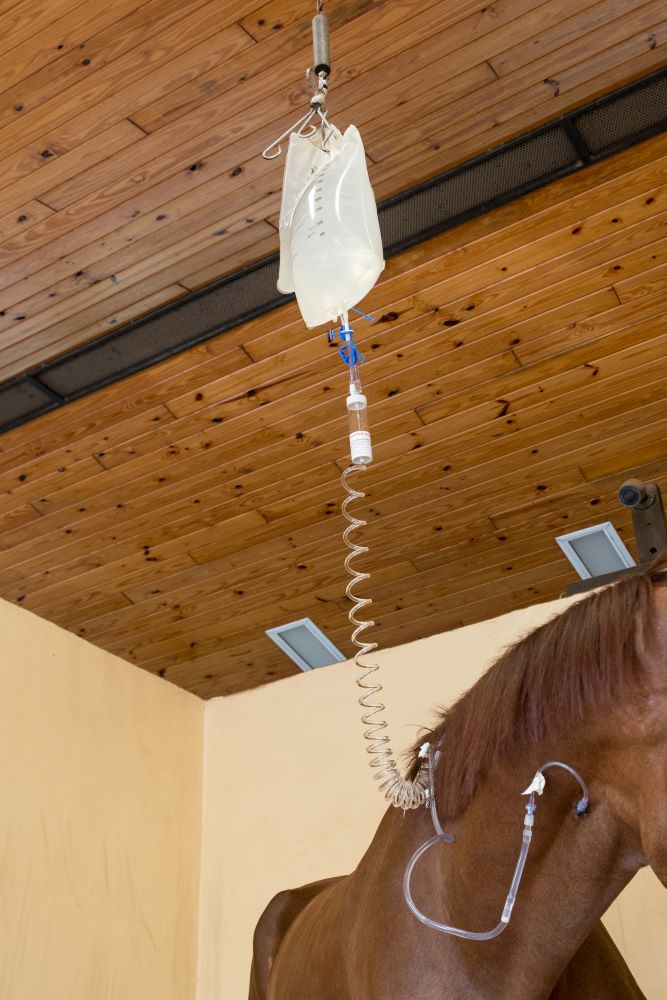
The next most important step is taking measures to either reestablish good flora within the gut or to remove the bad bacteria. In the past, a powdered charcoal was used, which is great for absorbing bacteria, but does not absorb the water. A gastrointestinal health supplement called BioSponge® came on the market in the early 2000s through the company Platinum Performance. The product is a purified clay powder that binds the toxins, and also binds the water, so that the horse loses fewer fluids in their equine diarrhea.
While absorbing the bad bacteria and toxins is important, also providing good bacteria in the form of probiotics can be very helpful.
“Probiotics are very variable in their efficacy, but there are some bacteria that are known to be associated with gut health,” Dr. Heidmann noted. “The good bacteria in people, and in horses, that has the most data for being helpful is Saccharomyces Boulardii. Old-fashioned brewers yeast is also Saccharomyces, but it is a different species, Saccharomyces cerevisiae.
“One of the best ways to re-establish healthy flora is Transfaunation, which is taking a healthy horses manure, filtering it, and then tubing it into the sick horse,” Dr. Heidmann added. “That is one of the most dramatic treatments out there. It provides the good ‘bugs’ that the horse is losing through the diarrhea. You will often see foals eating their mother’s manure. It is an instinctual habit to get the good bugs into their stomach. We only do that in the sickest of cases. Whatever the route, it makes a big difference to provide the good bugs because that creates the environment for the gut to heal.”
While some antibiotics are warranted in the right situation, Dr. Heidmann pointed out that they are not necessary as often as people would think.
“With people or dogs, if we get Salmonella or some other intestinal infection, we almost always go on antibiotics, but because antibiotics are the cause of many cases of colitis in horses, in general, that is not the best strategy,” Dr. Heidmann stated. “There are a couple of exceptions. Clostridium difficile does respond to antibiotics, metronidazole being the most common one. For Potomac Horse Fever, Tetracycline broad-spectrum antibiotics are the best.”
Biosecurity measures should also be taken to protect healthy horses from an infectious barn-mate. Dr. Heidmann recommends complete isolation of the sick horse while it is ill, and for a minimum of two full weeks after the infection has been clinically resolved. This includes no horse-to-horse contact, as well as no shared use of wheelbarrows, pitchforks, etc.
Molecular and DNA testing can be done to make sure that the horse is infection-free, however, Dr. Heidmann warns that testing can be problematic.
“There is a very high number of false negatives, meaning there is truly some infection there, but the lab cannot find it,” Dr. Heidmann stated. “There can be times when the horse is shedding bugs, but the tests do not pick it up. The state-of-the-art standard of care is a DNA test called ‘PCR’, and yet you still have to do multiple tests to get a positive test and get a diagnosis. Still, the best way to be safe is to continue testing until you are sure.”
Complications of Equine Diarrhea
Dr. Heidmann warned of common complications in severe diarrhea cases, laminitis being highest on the list. With the sickest of horses, it is unfortunately not uncommon for the veterinarian to get the gut fixed over three to five days, and then find that the feet have started to become very inflamed due to toxins in the bloodstream. If the horse loses the lining of its intestine, then the good and bad bacteria that are supposed to be contained in the intestine can “leak” out into the bloodstream and are free in the abdomen. Those bacteria are then dying either from an attack by the immune system or antibiotics, and they release endotoxins into the bloodstream, which along with other inflammatory products, can cause laminitis.
Another serious complication is blood clotting. The sick horse may become very low on blood protein when the bowel lining is damaged, which can cause clotting abnormalities. The horse may have difficulty clotting or they may become prone to abnormal increases in clotting. The horse might seem better, and then it will develop a clot somewhere in the body. It can be anywhere, but it is most often in the intestine itself, which is usually fatal. In general, horses like this are treated with supplemental protein in the form of plasma. In some cases, the veterinarian will also provide anticoagulant medications.

Although some cases of equine diarrhea are brief and easily resolved, Dr. Heidmann reminds that serious cases can go downhill fast, and it is important to refer to an expert.
“The biggest sign of a problem is duration,” Dr. Heidmann concluded. “If it is one day, it could be that they had a bite of bad food or something simple. If there are fevers or lethargy, those are instant warning signs. If it lasts for days, or if they go off their feed, those are instant warning signs. That is when you should call your veterinarian right away, especially because as they start to go downhill, these complications really amplify. The worst cases are the ones that have been smoldering for a day or two.”
Dr. Heidmann and the veterinarians at Palm Beach Equine Clinic are always available and encourage owners to contact the clinic at the first sign of a problem.
As one of the top equine medical centers, Palm Beach Equine Clinic has the pleasure of working with many highly specialized, world-class equine professionals. Dr. Peter Heidmann, DVM, DACVIM, is a Diplomate of the American College of Veterinary Internal Medicine, as well as the Owner/Hospital Director of Montana Equine Medical and Surgical Center in Three Forks, MT. In conjunction with a busy schedule of managing Montana’s leading full-service equine referral practice, Dr. Heidmann joined the team at Palm Beach Equine Clinic in Wellington, FL, for the first time this past winter to share his expertise in internal medicine. Dr. Heidmann is scheduled to return again for the 2017 winter season.
Dr. Heidmann grew up in New England and in the year 2000, graduated from Tufts University in Massachusetts with his veterinary degree. He completed his required internship at Arizona Equine, followed by a one-year surgical fellowship at Oregon State University. Beginning in 2002 to 2005, Dr. Heidmann completed a residency for Internal Medicine at the University of California, Davis.
Following his residency in 2005, Dr. Heidmann began his career with a private veterinary practice in Montana. Then an unfortunate turn of events quickly changed his new employment. Dr. Heidmann’s predecessor in Montana passed away in a tragic car crash on the last day of the year, and Dr. Heidmann stepped up to continue to build the practice left to him. Over the last ten years, Dr. Heidmann has developed Montana Equine to include two satellite offices and six senior veterinarians, plus become the leading referral hospital in the state.
As a Board Certified Internal Medicine Specialist, Dr. Heidmann specializes in neonatology, infectious disease, and ultrasound. In addition to his core internal medicine interests, Dr. Heidmann’s strengths also include advanced performance evaluations.
Dr. Heidmann was recruited by Dr. Scott Swerdlin, President of Palm Beach Equine Clinic, during the fall season of 2015. Dr. Heidmann’s wife, Allison, is a professional jumper and enjoys showing at the Winter Equestrian Festival (WEF). When Dr. Swerdlin offered Dr. Heidmann the opportunity to join PBEC and spend the winter in Wellington, he jumped at the opportunity.
“It worked out really well for me, for family reasons as well as professional reasons, to come down and do internal medicine specialty work during the winter in Wellington,” Dr. Heidmann detailed. “It is nice on the professional front, because Montana is the fourth biggest state, but the second lowest in per capita people. There are a lot of horses there, but there is not a lot of specialty horse work during the winter, so it was really nice to be able to work with the caliber of athletes that are at the WEF and come into Palm Beach Equine Clinic.”
“The facilities are really nice, and I am excited about the improvements they are making, because what was already there was incredible,” Dr. Heidmann said, pointing out recent renovations that are currently underway at the clinic. “It is great to have those resources at your fingertips, not just imaging and equipment, but the staff and variety of expertise. In Montana, I have six or seven veterinarians to bounce ideas off of, and all of a sudden at PBEC I had 30 people with different perspectives, and different backgrounds, and training. You get to see different ways of doing things and see how things can be done even more efficiently. I really emphasize the staff as much as the bells, whistles, and equipment.”
“There are not a lot of us Board Certified Internal Medicine veterinarians, because it is perceived as kind of an egghead, academic sub-discipline of equine work,” Dr. Heidmann admitted. “But what we focus on, especially in healthy horses like the athletes at WEF, are performance issues. Two of the most common, classic, performance-limiting issues in athletes, and especially in sport horses, are respiratory problems and muscle problems, which can range from quite subtle to severe.
“Muscles problems can be subtle issues that involve mild tweaking in diet or micronutrients, or they can be more severe issues like a horse that ties up,” Dr. Heidmann detailed, describing myopathy. “Similarly with respiratory problems, it can be a mild issue where the trainer or rider thinks that the horse used to be better or just is not performing up to its potential. It can be subtle respiratory problems like shortness of breath, or loud breathing, or slow recovery after work, or it can be more severe things like respiratory infections.”
Muscle issues and respiratory problems are the two main areas of internal medicine expertise, but the specialty can include many other things, such as liver problems, neurologic problems (brain and spinal cord both), and the care of sick neonates (foals).
“With seasonal breeders, that three-month period in Wellington is a high time for foals being born, and there is really a great deal that we can do with sick babies to end up with a healthy athlete in the end,” Dr. Heidmann noted. “Many people do not even realize what is possible with sick babies. It is possible to recover a top-notch performance horse out of a foal that looks quite dire.”
While Dr. Heidmann specializes in internal medicine, he and all of the veterinarians at Palm Beach Equine Clinic are very knowledgeable and experienced in general medicine practices.
“All of us in equine work are put in positions where we are generalists too, but what I really enjoy about being part of the team at PBEC is being able to focus on my true specialty,” Dr. Heidmann acknowledged. “This is what I spent so much time training to do, and to really be able to go in-depth, not just with the performance horses but non-WEF horses that are in the area as well, is a wonderful experience. We can really offer a level of treatment that is relatively rare in private practices.”
About Palm Beach Equine Clinic
The veterinarians and staff of Palm Equine Clinic are respected throughout the industry for their advanced level of care and steadfast commitment to horses and their owners. With 30 skilled veterinarians on staff, including three board-certified surgeons, internal medicine specialists, and world-renowned board-certified equine radiologists in the country, PBEC is known for leading the industry in new, innovative diagnostics and treatments. Palm Beach Equine Clinic provides experience, knowledge, availability, and the very best care for its clients. Make Palm Beach Equine Clinic a part of your team! To find out more, please visit www.equineclinic.com or call 561-793-1599.
More about Dr. Heidmann
Dr. Heidmann sees referrals and consults on cases from veterinarians throughout Montana and has served as an expert witness in many legal, welfare, and insurance cases. He served as the Internal Medicine Specialist for the 2011 Pan American Games in Guadalajara, Mexico, and participated as one of the founding veterinarians of Montana State University’s Bioregions program to Mongolia in 2014. He is Adjunct Faculty at Washington State University’s School of Veterinary Medicine in Pullman, WA, and Affiliated Faculty at Montana State University, Bozeman.