Tag: surgery
A horse was recently admitted to Palm Beach Equine Clinic (PBEC), based in Wellington, FL, with symptoms that included bleeding from the nostril. The patient’s referring veterinarian had diagnosed the horse with an ethmoid hematoma, which in layman’s terms is essentially a mass that fills with blood in the nose or sinus cavity.
The patient was placed under the care of PBEC’s board-certified surgeon Dr. Weston Davis and Dr. Michael Myhre. They performed an airway endoscopy to locate and evaluate the hematoma that the referring veterinarian had identified. After confirming the diagnosis, Dr. Davis and Dr. Myhre were eager to ensure that it was the one and only hematoma they were battling.
Computed Tomography
PBEC is one of an elite group of equine veterinary clinics to have a computed tomography (CT) machine in their arsenal of diagnostic imaging equipment. A CT gives veterinarians a unique look at the head, neck, and spine of a horse that they would never be able to accomplish with other imaging modalities. After a CT of the patient’s sinuses, more masses were indeed identified.
“This was a fairly typical presentation of an ethmoid hematoma, but there were certainly more masses than normal,” said Dr. Myhre. “It’s for this reason that the CT was very useful. If we were not able to obtain the scans that we did, we may have missed the masses that were located deeper in the sinus.”
The cause of an ethmoid hematoma is unknown, but the mass resembles a tumor in appearance and development without being neoplastic. Horses with extensive masses may have reduced airflow and an expanding hematoma can cause pressure necrosis of the surrounding bones, but rarely causes facial distortion. Treatments of the ethmoid hematoma can range from conservative management to surgery. The conservative treatment route includes the injection of formalin – a mixture of formaldehyde gas and water – into the mass using a guarded endoscopic needle. Once injected, the mass typically regresses rapidly, but recurrence is common. For some cases, surgical excision is achieved via a frontonasal bone flap procedure.
The Approach
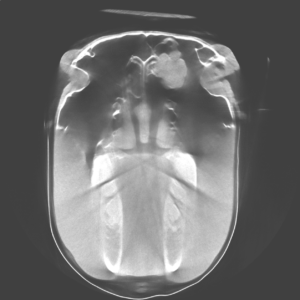
Due to the location and advances nature of the masses in this case, injection was not an option and the CT imaging was used to plan a surgical approach. “After sedation and a local block, we went into the sinus through a flap approach where we took a section of bone, cut it into a flap, and moved it back so we could go into the sinuses through a nice window,” said Dr. Myhre. “We removed a mass four centimeters in diameter as well as several smaller masses two to three centimeters in diameter, then flushed the area and closed.”
According to Dr. Myhre the advantages of a standing procedure included fewer risks from bleeding and fewer risks of recovering from anesthesia.
Post-surgery, the bone flap will require several weeks to heal, but the skin itself healed within one to two weeks, which is when the horse was cleared to return to normal activity.
Palm Beach Equine Clinic (PBEC) is changing the prognosis for condylar fracture injuries among sport horses. Advances in imaging, surgical talent, and the facilities necessary to quickly diagnose, treat, repair, and rehabilitate horses with condylar fractures have recently improved immensely.
Most commonly seen in Thoroughbred racehorses and occasionally polo ponies, a condylar fracture was once considered a career-ending injury. Today, however, odds are in favor of a full recovery with horses regularly returning to competition in their respective disciplines.
What is a Condylar Fracture?
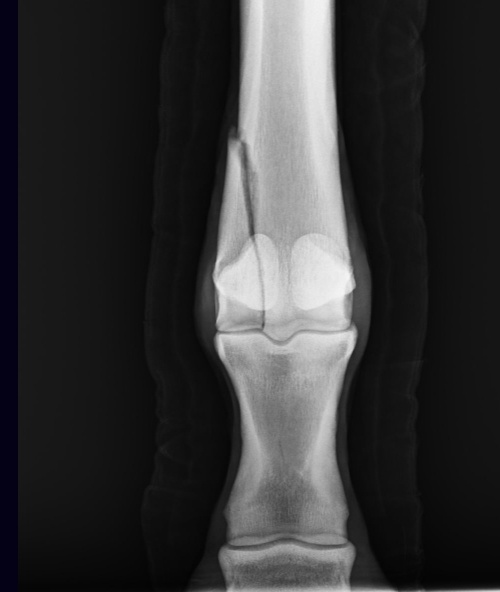
A condylar fracture is a repetitive strain injury that results in a fracture to the cannon bone above the fetlock due to large loads transmitted during high-speed exercise. 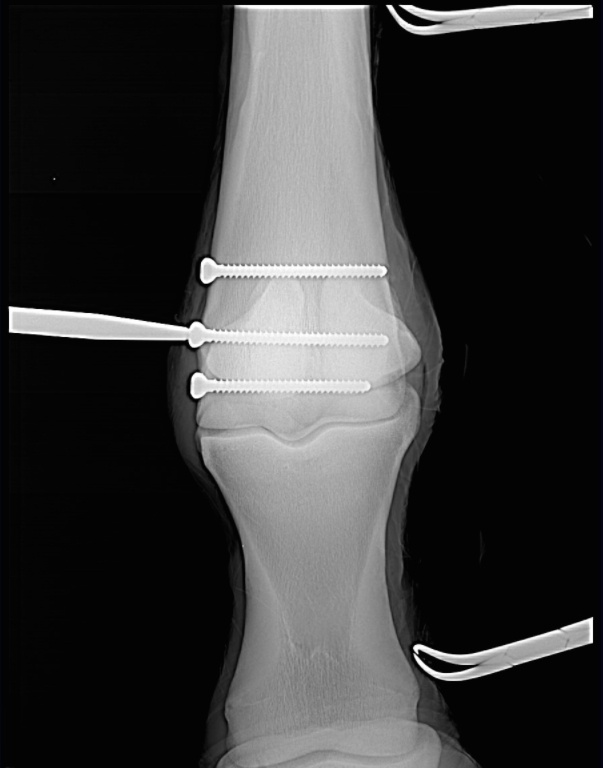
Scan showing the screws inserted during surgery (right). This patient, a Thoroughbred racehorse, walked away from surgery comfortably and is recovering well.
A condylar fracture is a repetitive strain injury that results in a fracture to the cannon bone above the fetlock due to large loads transmitted over the cannon bone during high-speed exercise. On a radiograph, a condylar fracture appears as a crack that goes laterally up the cannon from the fetlock joint and out the side of the bone, essentially breaking off a corner of the cannon bone, sometimes up to six inches long.
“A condylar fracture is a disease of speed,” said Dr. Robert Brusie, a surgeon at PBEC who estimates that he repairs between 30 and 50 condylar fractures per year. “A fracture to the left lateral forelimb is most common in racehorses as they turn around the track on a weakened bone and increased loading.”
Condylar fractures are further categorized into incomplete and non-displaced (the bone fragment hasn’t broken away from the cannon bone and is still in its original position), or complete and displaced (the fragment has moved away from the cannon bone itself and can often be visible under the skin).
Additionally, condylar fractures can occur laterally or medially. According to fellow PBEC surgeon Dr. Weston Davis, most condylar fractures tend to be lateral on the outside condyle (a rounded projection on a bone, usually for articulation with another bone similar to a knuckle or joint).
“Most lateral condylar fractures are fairly simple for us to fix,” said Dr. Davis. “Medial condylar fractures tend to be more complicated configurations because they often spiral up the leg. Those require more advanced imaging and more advanced techniques to fix.”
What is the Treatment?
The first step in effectively treating a condylar fracture through surgery is to accurately and quickly identify the problem. PBEC’s board-certified radiologist Dr. Sarah Puchalski utilizes the advanced imaging services at PBEC to accomplish exactly this.
“Stress remodeling can be detected early and easily on nuclear scintigraphy before the horse goes lame or develops a fracture,” said Dr. Puchalski. “Early diagnosis of stress remodeling allows the horse to be removed from active race training and then return to full function earlier. Early diagnosis of an actual fracture allows for repair while the fracture is small and hopefully non-displaced.”
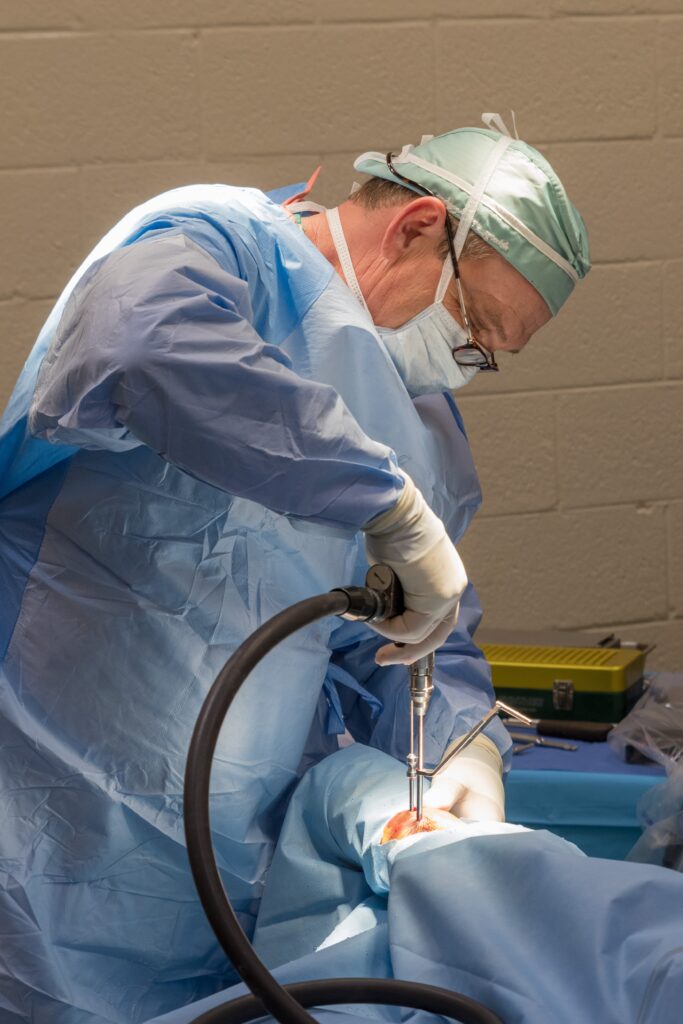
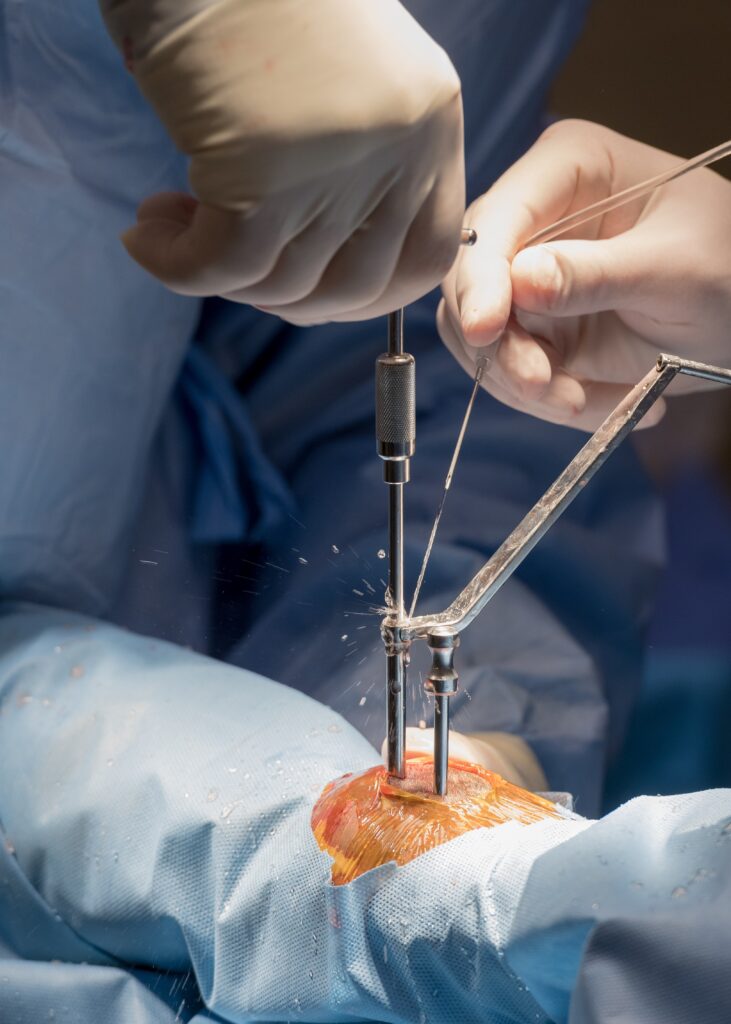
Once the injury is identified as a condylar fracture, PBEC surgeons step in to repair the fracture and start the horse on the road to recovery. Depending on surgeon preference, condylar fracture repairs can be performed with the horse under general anesthesia, or while standing under local anesthesia. During either process, surgical leg screws are used to reconnect the fractured condyle with the cannon bone.
“For a very simple and small non-displaced fracture, we would just put in one to two screws across the fracture,” explains Dr. Davis. “The technical term is to do it in ‘lag fashion,’ such that we tighten the screws down heavily and really compress the fracture line. A lot of times the fracture line is no longer visible in x-rays after it is surgically compressed. When you get that good compression, the fractures heal very quickly and nicely.”
More complicated fractures, or fractures that are fully displaced, may require more screws to align the parts of the bone. For the most severe cases of condylar fractures, a locking compression plate with screws is used to stabilize and repair the bone.
PBEC surgeon Dr. Jorge Gomez, approaches a simpler non-displaced condylar fracture while the horse is standing, which helps to aid in a faster recovery and more successful surgical outcome.
“I will just sedate the horse and block above the site of the fracture,” said Dr. Gomez. “Amazingly, horses tolerate it really well. Our goal is always to have the best result for the horse, trainers, and us as veterinarians.”
According to Dr. Gomez, the recovery time required after a standing condylar fracture repair is only 90 days. This is made even easier thanks to a state-of-the-art surgery pit installed at PBEC. The four-and-a-half-foot recessed area allows doctors to perform surgeries on anything from a horse’s hock and below from a standing position. Horses can forgo the risks of general anesthesia for a mild sedative and local nerve blocks, greatly improving outcomes.
“A condylar fracture was once considered the death of racehorses, and as time and science progressed, it was considered career-ending,” concluded Dr. Brusie. “Currently, veterinary medical sciences are so advanced that we have had great success with condylar fracture patients returning to full work. Luckily, with today’s advanced rehabilitation services, time, and help from mother nature, many horses can come back from an injury like this.”
Success Story: Ameloblastic Fibroma
When a middle-aged mare with a mysterious mass in her mouth came under the care of Palm Beach Equine Clinic in Wellington, FL, Dr. Weston Davis pulled out all the stops to find a definitive diagnosis. The oral mass was growing at a rapid rate and was positioned just behind the bottom incisors on the left bar of the horse’s mouth.
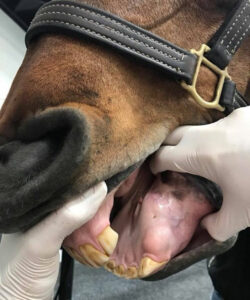
A view of the oral mass being examined by Dr. Davis.
Computed Tomography Imaging
First, Dr. Davis turned to the use of PBEC’s state-of-the-art computed tomography (CT) machine to obtain an image of the mass and its exact location within the horse’s mouth. Then, a surgical biopsy was performed and the histopathology, or microscopic examination of the biopsied tissue, revealed the manifestation of an ameloblastic fibroma. An ameloblastic fibroma is a mixed odontogenic (dental) tumor composed of soft tissues.
“Although this tumor type rarely metastasizes, it tends to be locally invasive and aggressive, requiring the complete removal and/or aggressive radiation therapy,” said Dr. Davis, who is a board-certified surgeon at PBEC.
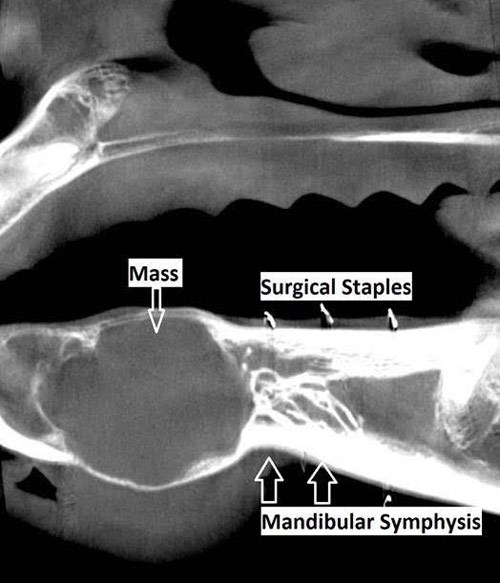
Ameloblastic Fibroma Treatment Plan
A tumor of dental origin is rarely found in humans and is extremely rare in equines, but upon diagnosis, Dr. Davis quickly identified a treatment plan, saying, “In this case, the CT mapping that was performed enabled us to completely remove the tumor via a rostral mandibulectomy with preservation of the mandibular symphysis (the joint between the two halves of the mandible).”

The horse underwent surgery at PBEC and Dr. Davis removed the tumor along with the rostral (front) mandible, which includes the lower incisor teeth and essentially the entire front portion of the lower jaw of the horse.
The obvious question that arises from a rostral mandibulectomy is “how effectively will the horse be able to eat without bottom teeth?” For this patient, however, the answer came quickly and it was nothing short of encouraging. The mare returned to eating just hours after surgery and, at her two-week checkup with Dr. Davis, was back on a normal diet of hay, grain, and – of course – treats.
According to Dr. Davis, the majority of animals that undergo this type of surgery often compensate well and have little trouble eating. For this mare, her only struggle in the future may be the prehension of very short and/or tough pasture.

A view of the lower lip of the horse after surgery. 
Two weeks post-surgery and no visible signs of a rostral mandibulectomy.
Post Mandibulectomy Surgery
Also at two weeks post-surgery, Dr. Davis approved the mare for light riding activity with a hackamore. The mare competed in the jumper ranks before surgery and at a four-week checkup, Dr. Davis gave the all-clear and the mare returned to full work. She even made a comeback in the competition ring at Palm Beach International Equestrian Center with very little visual evidence that a mandibulectomy was ever performed.
“This was a rare tumor and a rare surgery, but the horse recovered incredibly well and fast!” said Dr. Davis. “It was an excellent patient outcome. “I gave her the all-clear at four weeks post-surgery and she is already back to winning classes.”
All Photos Courtesy of Dr. Weston Davis
Any horse owner’s worst nightmare is realized when their mount begins to show the dreaded signs of colic. For Jody Stoudenmier, a Wellington, FL, resident and avid dressage rider, she knows the symptoms all too well.

Patient History
Stoudenmier owns an 11-year-old American-bred Dutch Warmblood mare that joined her string of horses at the end of 2016 and has competed through the Intermediate II level. Sidelined by a suspensory injury last year, Beatrix was prescribed stall rest to aid in her recovery by Dr. Robert Scott of Scott Equine Services based in Ft. Lauderdale, FL. An unfortunate but common side effect of the necessary stall rest was colic. Beatrix suffered from six bouts of colic that were resolved without surgery when Dr. Scott referred Stoudenmier and Beatrix to Palm Beach Equine Clinic.
“She is such a wonderful mare; a nice mover, very athletic, sweet, sensitive, and easy to handle in the barn,” said Stoudenmier of the mare that regularly competes at the Adequan Global Dressage Festival during the winter season. “When she was recovering from her injury we tried everything to prevent her from colicking – diet, medications, hand walking – but, nothing seemed to be working.”
It was then that Palm Beach Equine Clinic’s board-certified surgeon, Dr. Weston Davis, suggested a laparoscopic surgical approach.
“Her colic had never progressed so far that we needed to do surgery before,” explained Stoudenmier. “But, at that point, I was open to anything! After speaking with Dr. Davis, I immediately had a positive feeling about it.”
Dr. Davis’ Surgical Procedure
The procedure that Dr. Davis suggested was an endoscopic ablation of nephrosplenic space. In layman’s terms, as a result of Beatrix’s colic, her colon was essentially getting caught or entrapped over the nephrosplenic ligament, which connects the left kidney to the spleen. When the colon is entrapped in this position, its contents cannot move through it and the colon becomes distended, causing the horse considerable pain, and the inevitable colic.
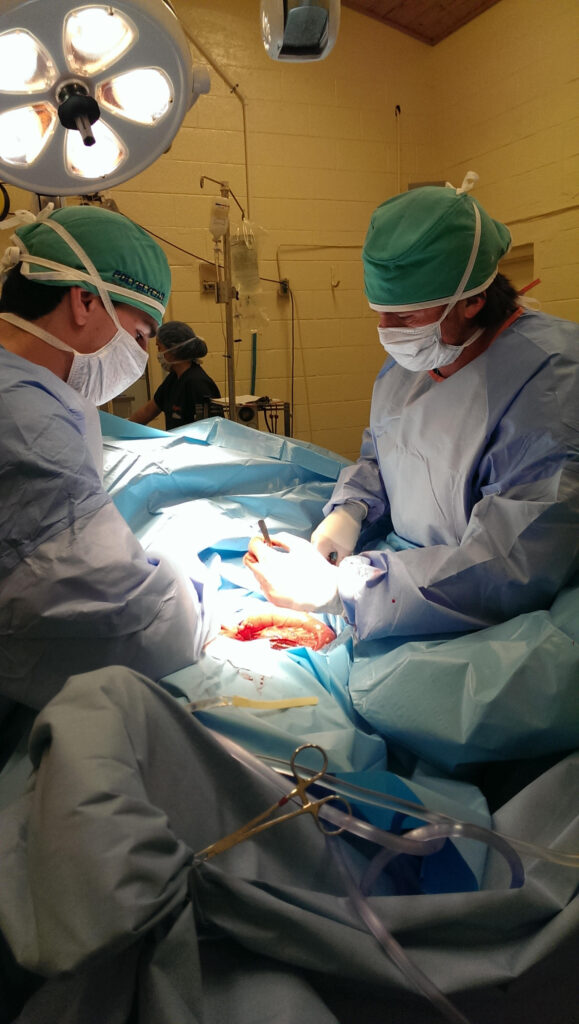
Dr. Davis’ solution was to close or perform an ablation of the nephrosplenic space to prevent further entrapment. The procedure can be conducted endoscopically where the horse does not have to be anesthetized, but undergoes a standing surgery with sedation and local anesthesia. A small incision is made in the left flank and the laparoscope is inserted through a smaller incision close by. The nephrosplenic space is then sutured closed so that the trough that forms the space between the kidney and spleen is obliterated and can no longer entrap the colon.
On October 9, 2017, Beatrix underwent a successful ablation of the nephrosplenic space at the hands of Dr. Davis.
“In the past, I have had several horses undergo surgery where they had to be anesthetized and it was very difficult to get them standing again after surgery,” said Stoudenmier. “We did not have that worry with Beatrix and the approach absolutely made a difference in her recovery.”
Post-Surgery Care and Recovery
Beatrix remained at Palm Beach Equine Clinic for a week and a half after surgery to jump-start her recovery before returning home to Stoudenmier, who has managed her post-surgery care with the help of both Dr. Davis and Dr. Scott.
“Dr. Davis was absolutely wonderful to work with,” said Stoudenmier of her experience at Palm Beach Equine Clinic. “He listened to my concerns, was patient, and kept his mind open.”
Dr. Davis paid a visit to Beatrix in mid-November to perform an ultrasound and together with Dr. Scott approved the mare to return to work. Stoudenmier has begun to introduce trot work into Beatrix’s routine and is optimistically expecting a full recovery, saying, “She looks super and everything looks good for the next two months. My goal by the end of the season is to get her back in the show ring!”
Success Story: Freeman
In January 2016, the Pine Hollow team noticed something seemed off just before driving out of the Winter Equestrian Festival (WEF) with their horses. Stopping to check the horses before continuing off the showgrounds, Pine Hollow discovered Freeman, a promising and successful Dutch Warmblood, had swung his hind leg over the back of the trailer. Freeman’s stifle had ended up squarely on one of the hooks used to secure the back door, lodging the hook into his stifle and into the femoropatellar joint.
Emergency Veterinary Care
Recognizing the extreme peril facing Freeman, Pine Hollow immediately called for help from Palm Beach Equine Clinic, the Official Veterinarians of WEF.
“It took tremendous effort, creative thinking, and exceptional teamwork to free Freeman from the hook impaling his leg,” said David Blake, Pine Hollow’s internationally acclaimed rider and trainer. “Palm Beach Equine Clinic sent several of their top vets to help us rescue Freeman. The team of vets is truly great.”
Thanks in very large part to the help and determination of the vets, Pine Hollow and Palm Beach Equine Clinic were able to free Freeman from the trailer door.
At the Equine Hospital
From there, Freeman was transported to the nearby Equine Hospital, where he spent a few days recovering before it was agreed to pursue arthroscopic surgery on his femoropatellar joint.
“To be honest, it wasn’t looking good at all for the first day or so Freeman was there,” said Blake. “The joint was so severely damaged we didn’t know if it could be fixed. Our only chance of fixing the joint was surgery, so we agreed we would try everything possible.”
Dr. Weston Davis performed the surgery, after which Freeman remained in Palm Beach Equine Clinic’s care while he regained use of the leg.
“The team did a fantastic job there and kept Freeman until he was ready to begin long-term rehab with James Keogh,” said Blake.
When Freeman was finally ready to return home to Pine Hollow, Blake hoped at best Freeman would eventually be able to do light work and perform at a low level.
At Palm Beach Equine Clinic in Wellington, FL, the team of Board-Certified surgeons are experts in minimally invasive surgical techniques, aiming to reduce joint disease, resolve lameness, and improve the longevity of sport horse careers.
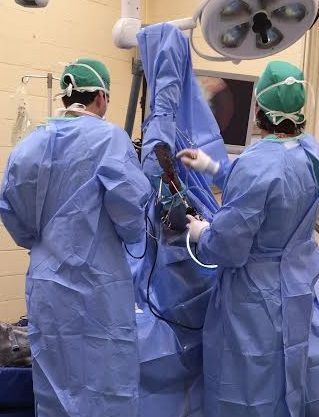
Arthroscopy (or arthroscopic surgery) is a minimally invasive surgical technique that can be performed on an injured joint or synovial structure to accurately explore and treat pathology. The surgery generally involves two very small (8mm) keyhole incisions. The first incision is where the surgeon will insert the arthroscope, which is an instrument with a small surgical grade camera installed that allows a complete, clear view of the interior joint surface. The second small incision is created to insert the surgical instrument to perform the procedure.
Arthroscopy is used to treat a broad range of injuries inside of a joint. Chip fracture removal is a procedure that is particularly commonly in both young Warmblood horses with developmental disease and in racehorses travelling at high speeds. A small chip fracture can cause persistent irritation in the joint as well as arthritis if left untreated. It is best removed immediately so that no further damage is created. The surgeon can go into the joint, remove the chip, and clean up the surrounding cartilage. Most horses recovery quickly and return to their normal athletic activity.
Board-Certified Surgeon Dr. Weston Davis performs many arthroscopic surgeries at Palm Beach Equine Clinic alongside fellow surgeons Dr. Robert Brusie and Dr. Jorge Gomez.
“In many horses, we consider arthroscopy as a prophylactic measure, intervening after injury, but before the development of a generalized degenerative arthritic cycle ensues,” Dr. Davis stated. “Arthroscopy is definitely something that you want to do early in the game if you feel like the horse has joint disease, or a chip, or cartilage disease, or an undefined injury that is not responding appropriately to medical therapy. Arthroscopy can be curative for some of these horses. But if you do not intervene early on in the course of the disease and there is already advanced arthritis, then you have missed your window.
“Arthroscopy is a preferred treatment because it is minimally invasive so most horses can go right back to work,” Dr. Davis continued. “In a typical scenario, we thoroughly explore the joint with the arthroscopic camera, we remove a chip or repair a lesion, and the horse is not lame after the surgery. Because of the small incisions, there is minimal aftercare and horses are often able to go back to work quickly.”
Other common indications for arthroscopic surgery are meniscal disease in the stifle, subchondral cystic lesions, primary cartilage lesions, and debridement of damaged tendinous/ligamentous tissue (such as deep digital flexor tendon tears in the navicular bursa). The surgeons at Palm Beach Equine Clinic can perform arthroscopy on virtually any joint in the horse. Anything from the Temporomandibular Joint (TMJ) of the head to the navicular bursa within the hoof capsule can be explored and treated with this minimally invasive approach.
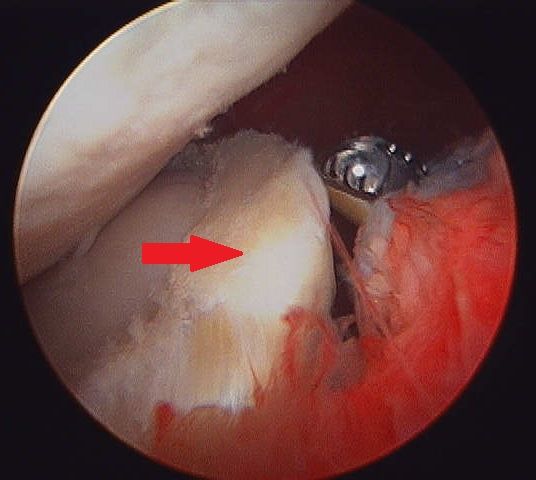
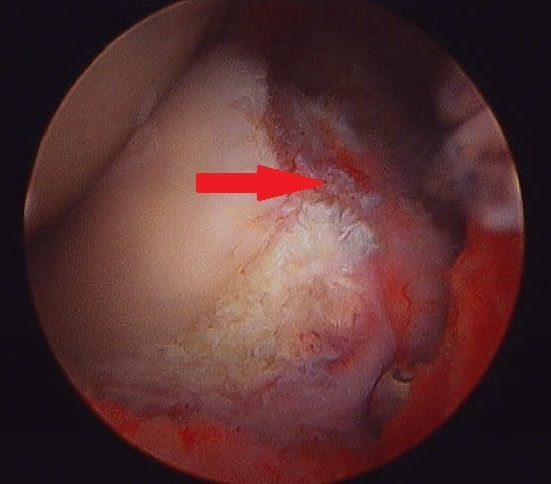
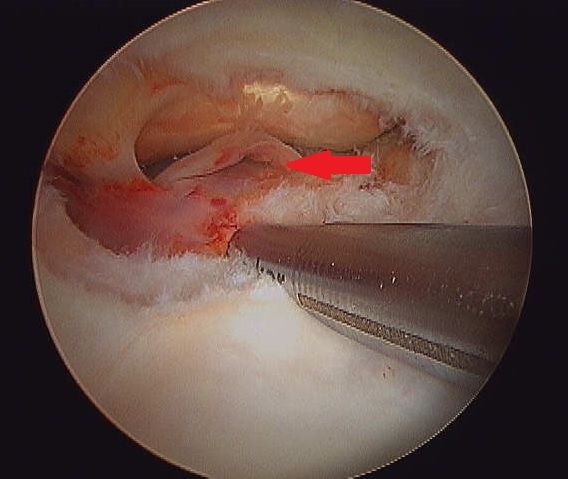

Almost all arthroscopies are performed under general anesthesia with the horse on its back. New renovations at Palm Beach Equine Clinic include a set of stocks of adjustable height adjacent to a surgeon’s pit, allowing the surgeons to have eye-level access to the joint they are working on, enabling many new procedures on the legs of standing horses.
Minimally invasive surgery allows for a simple and quick recovery for the horse. The traditional horse would be on stall rest with a bandage on until the sutures come out at two weeks, and then start doing some light hand walking and physical therapy. Barring severe damage in the joint or associated tendon/ligament disruption, most cases will undergo a six-week rest and rehabilitation protocol, then return to normal work.
As always, the advanced diagnostic imaging at Palm Beach Equine Clinic permits the surgeons to get a complete evaluation of an injury involving a joint to ensure the best possible outcome. Depending on the injury type, digital radiographs, ultrasound, MRI, and Nuclear Scintigraphy, or a combination thereof, may be used for pre-operative diagnosis and planning. Ultrasound and digital radiography are available for intra-operative use. Intra-operative CT scanning will also be available in the future with the new additions at Palm Beach Equine Clinic.
“When you are inside the joint with an arthroscopic camera, you have the most complete picture of the surface and health of that joint,” Dr. Davis noted.
Palm Beach Equine Clinic (PBEC), located in Wellington, FL, offers advanced diagnostic imaging, world-renowned surgical talent, and state-of-the-art facilities necessary to quickly diagnose, treat, and repair horses with condylar fractures, making PBEC one of the leading facilities in the U.S. for condylar fracture repairs.
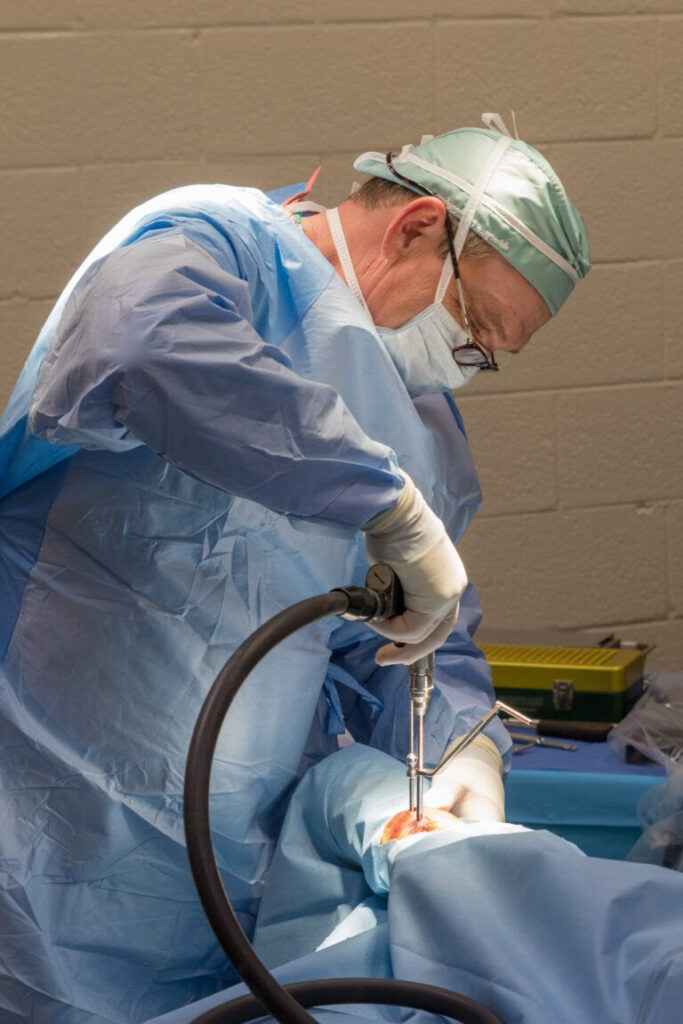
With thanks to the technology required for early diagnosis and experienced surgeons on staff, horses that are admitted to PBEC for condylar fracture repairs are more likely to return to training quickly. Most commonly seen in Thoroughbred racehorses and occasionally polo ponies or eventing horses, a condylar fracture was once considered a career-ending injury. Today, however, advances in technology aid in a full recovery with horses regularly returning to competition in their respective divisions.
What is a Condylar Fracture?
A condylar fracture is a repetitive strain injury that results in a fracture to the cannon bone above the fetlock due to large loads transmitted during high-speed exercise. On a radiograph, a condylar fracture appears as a crack that goes from the fetlock joint up the cannon bone. Lateral fractures many times exit the bone usually one-third of the way up the bone. Medial fractures will oftentimes spiral up to the hock or knee. Medial fractures are much more common in the hindlimb than the forelimb. It is the spiral fractures that are more difficult, due to the fact that the extent of the spiral cannot be identified radiographically. If the surgeon cannot identify the fracture, then that part of the fracture cannot be repaired.
“A condylar fracture is a disease of speed,” said Dr. Robert Brusie, a surgeon at PBEC who estimates that he repairs between 30 and 50 condylar fractures per year. “A fracture to the left lateral forelimb is most common in racehorses as they turn the track on a weakened bone and increased loading on the lateral condyle.”
Condylar fractures are further categorized into two classes. An incomplete and non-displaced fracture means that the bone fragment is not separated from the cannon and is still intact with its original position. A complete and displaced fracture means the fragment has detached from the cannon bone and this fracture can often be visible under the skin. Displaced condylar fractures have a somewhat lower prognosis due to the fact that soft tissue structures, such as the joint capsule, become torn. When these structures heal, they are thicker, which makes the joint less flexible.

“Most lateral condylar fractures are fairly simple for us to fix,” said PBEC surgeon Dr. Weston Davis. “Medial condylar fractures tend to be more complicated configurations because they often spiral up the leg. Those require more advanced imaging and more advanced techniques to fix.”
What is the Treatment?
The first step to effectively treating a condylar fracture through surgery is to accurately and quickly identify the problem. PBEC’s Board-Certified Radiologist Dr. Sarah Puchalski utilizes the advanced imaging services at PBEC to assist in the diagnosis.
“Stress remodeling can be detected early and easily on Nuclear Scintigraphy before the horse goes lame or even develops a fracture,” said Dr. Puchalski. “Early diagnosis of stress remodeling allows the horse to be removed from active race training and then return to full function earlier. Early diagnosis of an actual fracture allows for repair while the fracture is small and hopefully non-displaced.”
Once identified as a condylar fracture, PBEC surgeons step in to repair the fracture and start the horse on the road to recovery. Depending on surgeon preference, condylar fracture repairs can be performed with the horse under general anesthesia, or while standing under local anesthesia and sedation. During either process, surgical lag screws are used to reconnect the fractured condyle with the cannon bone.
“For a very simple and small non-displaced fracture, we would just put in one to two screws across the fracture,” explains Dr. Davis. “The technical term is to do it in ‘lag fashion’, such that we tighten the screws down heavily and compress the fracture line. Many times the fracture line is no longer visible in x-rays after it is surgically compressed. When you achieve good compression, the fractures heal very quickly and nicely.”
More complicated fractures, or fractures that are fully displaced, may require more screws to align parts of the bone. For the most severe cases of condylar fractures, a locking compression plate with screws is used to stabilize and repair the bone.
Severe condylar fractures often require general anesthesia, but for PBEC surgeon Dr. Jorge Gomez, approaching a simpler non-displaced condylar fracture while the horse is standing helps to aid in a faster recovery and successful surgical outcome.

“I think it takes the risk of anesthesia away and is a faster surgery from the time the horse comes in to the time the horse recovers,” said Dr. Gomez. “I will just sedate the horse and block above the site of the fracture. Amazingly, horses tolerate it really well, and it is very convenient for medial condylar fractures. In these cases, the fracture can spiral all the way up through the cannon bone, and they have a tendency to develop complete catastrophic fractures that can happen at any time after the injury. That risk can be significantly increased by the recovery from general anesthesia. Our goal is always to have the best result for the horse, trainers, and us, as veterinarians.”
According to Dr. Gomez, the recovery time required after a standing condylar fracture repair is only 90 days.
While Dr. Brusie, Dr. Davis, and Dr. Gomez are all seasoned in quickly and effectively repairing condylar fractures, PBEC is helping them to stay on the cutting edge of surgical techniques. PBEC is currently renovating its facility with plans to give surgeons a new approach to fix condylar fracture repairs. A set of stocks and surgeon’s pit have been added with the ability to give the surgeon eye-level access to the fracture with the patient standing and subsequently simplifying the procedure by reducing the risk from recumbent recovery.
What is the Prognosis?
One of the most common questions regarding an equine injury is, “Will the horse return to work?” Thanks to advanced imaging and surgical techniques, the answer to that question when involving a condylar fracture is most likely, “Yes.” At PBEC, a condylar fracture diagnosis rarely results in the end of a racehorse’s career.
Diagnostic imaging plays a major role in assisting to diagnose, surgically map, and follow up on condylar fractures. After primary use to diagnose a condylar fracture, digital radiographs are also used after surgery to ensure that a fracture repair was completely successful. According to Dr. Davis, scanning two planes during and after surgery gives a full view of the fracture and repair techniques, immediately indicating the success of the procedure before moving the horse on to recovery.
“A condylar fracture was once considered the death of racehorses, and as time and science progressed, it was considered career-ending,” said Dr. Brusie. “Currently, veterinary medical sciences are so advanced that we have had great success with condylar fracture patients returning to full work. Luckily, with today’s advanced rehabilitation services, time, and help from mother nature, many horses will come back from an injury like this.”
Palm Beach Equine Clinic provides experience, knowledge, availability, and the very best care for its clients. Make Palm Beach Equine Clinic a part of your team!
Palm Beach Equine Clinic of Wellington, FL, is a worldwide leader in sport horse medicine and emergency colic care. While symptoms of colic should be treated medically first, surgical intervention can be necessary, and the team at Palm Beach Equine Clinic is prepared for every situation.
With three Board-Certified Surgeons on staff, as well as a state-of-the-art hospital and the most advanced surgical equipment, Palm Beach Equine Clinic has a very high success rate in saving horses from life-threatening colic. The veterinarians take pride in their equine clients returning to full intended use and continuing to perform at their highest levels.
Causes and Symptoms
Colic is defined as any source of abdominal discomfort in the horse. Abdominal pain or problems within the gastrointestinal tract can arise unexpectedly from many different origins, including but not limited to: spoiled feed, abrupt changes in feed, parasite infestation, sand ingestion, lack of water consumption, excess stress, or changes in the weather. Many times there is not a well-defined inciting cause.
The most important step any owner can take is to recognize the symptoms as early as possible and immediately call their veterinarian. Pawing, rolling, looking at the abdomen, sweating, loss of interest in food and water, and absence of gut sounds in any of the four quadrants are common symptoms. The sooner the veterinarian gets involved in treatment, the better the horse’s chance of survival.
In the event of an emergency, the surgeons and veterinarians of Palm Beach Equine Clinic are available 24/7. When an equine patient is admitted to the hospital, every step is taken to quickly diagnose the problem and correct it immediately.
Tests and Diagnosis
Board-Certified Surgeon Dr. Weston Davis explained that one of the biggest challenges in the sport horse population is determining surgical versus non-surgical colic cases.
“We do not want to put a non-surgical case through the risk of anesthesia and the months of healing time, so we try to spare that at all costs and determine the surgical cases as accurately as we can,” Dr. Davis detailed. “On the split side of that, we try to operate as quickly as possible on any horse that needs surgery and not miss any surgical lesion types.”
There are several methods for differentiating surgical cases. Simple physical exam findings, such as the color of the gums, heart rate, gut sounds, and level of pain can all be supportive of surgical necessity. A variety of tests may also include abdominal ultrasounds and rectal exams.
An Abdominocentesis (or belly tap) is performed on every questionable colic case, where fluid is collected from around the intestines and analyzed for color and character. A variety of other laboratory tests will be run on the fluid as well, with the aim of quickly determining if the horse’s bowel is compromised.
Surgical Procedures
If surgery is necessary, there are a few different approaches that may be performed depending on the specific case.
For chronic colic cases, such horses with longstanding, intermittent colic, an abdominal exploratory procedure may be done with laparoscopy. This option can be done with the horse standing and is a minimally invasive way to examine the full abdomen.
In most acute cases, further steps must be taken. If the veterinarian determines that the horse is a surgical candidate, the patient will go under general anesthesia. The surgeons try to make as small of an incision as they can to perform the needed surgical correction.
“If we intervene early, we can take a strangulating or compromised lesion – one that most people understand as a twist – and we can go into the abdomen and correct the twist, reposition everything appropriately, explore the remainder of the abdomen to make sure nothing else is going on, and then close them up,” Dr. Davis explained. “Some of these surgeries can be as quick as 30 minutes and require just an untwisting, repositioning, and closure. The ones that are bad are the usually the cases that have a more severe twist or have been going on longer.”
In more severe or long-standing cases, the surgery can require a resection and an anastomosis procedure to excise a compromised or devitalized segment of the intestine. The surgeon then joins the healthy ends back together.
“Even more advanced procedures would be like a re-plumbing of the intestines,” Dr. Davis noted. “One of the most common examples of this would be a patient with damage to the end of the small intestine, near or involving its junction with the cecum. In a case like this, we would perform a ‘jejunocestomy’ where we join another part of the small intestine to a different position on the cecum.”
Post-Operative Recovery
After any surgery, there is a process of recovery, which Palm Beach Equine Clinic makes as easy as possible for its clients. In the traditional recovery, most horses will remain in the hospital for a few days. In the post-operative period, they generally receive fluids until they are ready to eat and drink, 3-5 days of antibiotics, and 5-7 days of anti-inflammatories.
“The recovery process is highly dependent upon how sick they are after surgery,” Dr. Davis stated. “Some horses will bounce back and be home 48 hours later, but a very sick horse could potentially spend seven to ten days in the hospital until they are healthy enough to get off fluids and go home.”
After leaving the hospital, the horse is usually placed on one month of stall rest, followed by another month of turnout in a small paddock. In between eight to 12 weeks, the horse will usually be fully recovered and ready to start back to work.

Physical Therapy
With the sport horse in mind, PBEC pays special attention to the health of the abdomen following surgery. The health of the abdominal incision and prevention of infection or hernias is very important. In most cases, the surgeon will recommend physical therapy and special exercises to re-strengthen the horse’s abdominal muscles so that it can get back to work quickly and have a strong abdominal musculature when it does.
“Making the horse walk backwards is one thing that will make them tighten and work their abdominal musculature,” Dr. Davis shared. “Pinching or tickling around their tail head is another common exercise to make them do something similar to a stomach crunch.”
As one of the top equine emergency care centers in the world, Palm Beach Equine Clinic is prepared to handle any case, 24 hours a day, seven days a week, and 365 days a year.
“With the combination of quick surgical intervention, excellent surgical care, and specialized post-operative measures, Palm Beach Equine Clinic has a very high rate of return to athletic performance for all of our colic cases,” Dr. Davis concluded.
Palm Beach Equine Clinic provides experience, knowledge, availability, and the very best care for its clients. To find out more, please visit www.equineclinic.com or call 561-793-1599.
Palm Beach Equine Clinic is proud to serve as the local headquarters for emergency services and equine diagnostics during the winter show season in Wellington, FL. As the official veterinary hospital of the Winter Equestrian Festival (WEF) and the Adequan® Global Dressage Festival (AGDF), Palm Beach Equine Clinic has been the premier surgical facility in Wellington for over three decades.
While competing in South Florida, horses and riders from around the globe have access to Palm Beach Equine Clinic’s state-of-the-art hospital for all of their sport horse needs. Palm Beach Equine Clinic has a team of over 30 veterinarians, which includes three Board-Certified Surgeons, a Board-Certified equine Radiologist, and numerous other experts in their fields. All competitors and their traveling veterinarians are welcome for the support of services and collaboration throughout the season.
Referral Veterinarians Welcome
The referring relationship between veterinarians is most commonly seen in the specialty departments of surgery, internal medicine, ophthalmology, and advanced diagnostic imaging. At Palm Beach Equine Clinic, the advanced diagnostic imaging and surgical technology is unmatched, and the three Board-Certified Surgeons are skilled in many procedures that require high levels of expertise and advanced current equipment. As a result, many veterinarians refer their clients to the facility for specialty services.
Dr. Weston Davis, one of the Board-Certified Surgeons on the staff at Palm Beach Equine Clinic, works with many referral cases. Throughout the year, veterinarians from all over Florida frequently refer their clients to Palm Beach Equine Clinic for surgical procedures and advanced diagnostic imaging. The referring veterinarians may range anywhere from general practitioners to other surgeons that do not have access to surgical facilities or the most modern diagnostic imaging modalities while on the road.
“As a rule, we are friendly with referring doctors and take care of their clients with as much high-level care and professionalism as possible,” Dr. Davis stated. “It is important to us to maintain good relationships with the veterinarians that refer to us for specialty work. We always try to facilitate whatever level of involvement they desire. If they want to come and be there for the surgical procedure, we make that happen, and if they just want to send the case and not be as involved, we can do that as well. However, we also always collaborate with the referring veterinarian and the client as a team. If they send a horse in for a surgical procedure, we are going to do the procedure and then connect the client with the referring physician for the follow-up.”
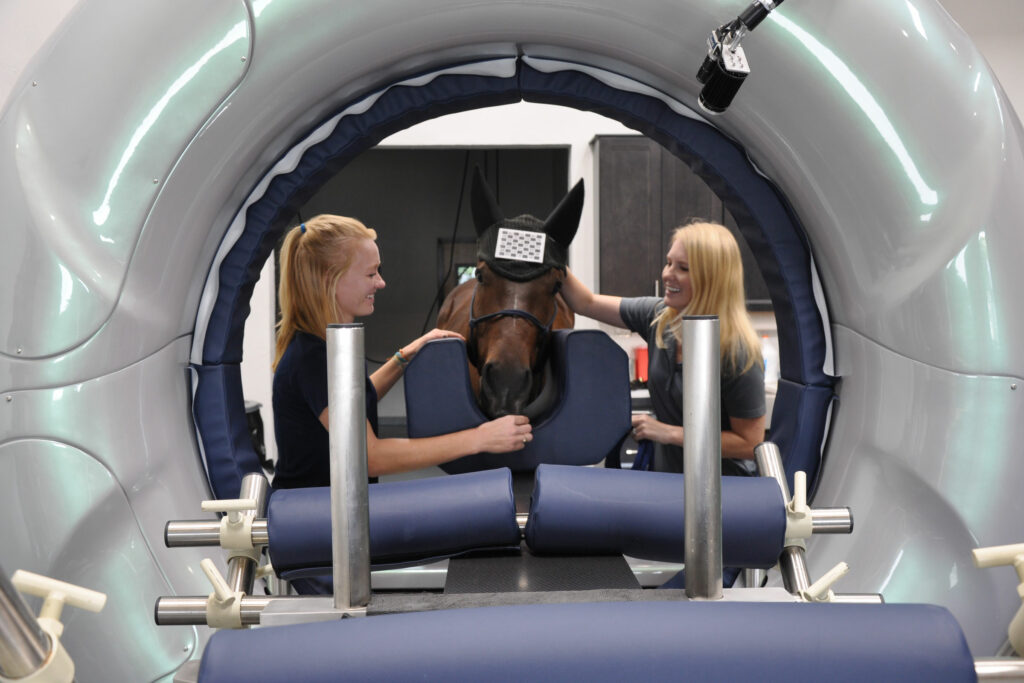
Talented Surgeons and Advanced Diagnostic Imaging
The cutting-edge services available at Palm Beach Equine Clinic are made possible by the expertise of the hospital’s talented surgeons, along with the assistance of state-of-the-art diagnostic imaging and comprehensive surgical and medical resources. The combination brings many of the best veterinarians in the world to Palm Beach Equine Clinic for assistance with their most complex cases.
Among the hospital’s features, the latest in surgical technology enables less invasive operations that result in faster recovery times for the horse. Dr. Davis explained how diagnostic imaging is used during surgery to help guide procedures and assure the best possible result.
“Magnetic Resonance Imaging (MRI) and other advanced diagnostic imaging modalities can often be used for three-dimensional mapping to help enhance the surgical technique,” he noted. “There are some fractures in particular where the surgeon can map out the exact configuration of the fracture off of the MRI scan. We are then able to place markers with the MRI to guide a more exact, refined surgery.
“Intra-operatively, x-rays are taken to view progress, particularly for fracture repairs,” Dr. Davis continued. “The digital radiographs allows us to view the fracture in two planes to ensure optimal screw placement and fracture repair. Ultrasound is also frequently used in surgery for some of the more delicate procedures, specifically with soft tissue.”
Other surgical procedures may be guided with Arthroscopy, which aids in visualization of a joint; Laparoscopy, which uses a camera inserted into the abdomen; or Endoscopy, which is used in upper airway procedures. With the most advanced diagnostic imaging technology onsite, Palm Beach Equine Clinic is the go-to hospital for equine owners and referral veterinarians from around the world during the winter season in Wellington.
Palm Beach Equine Clinic provides experience, knowledge, availability, and the very best care for its clients. Make Palm Beach Equine Clinic a part of your team! To find out more, please call 561-793-1599.
Jo Ann Hopkins and her 12-year-old Appendix-bred gelding, Blazer, were placed third in points in their local 1D barrel racing circuit. However, three months earlier, Blazer underwent surgery at Palm Beach Equine Clinic for a growing cyst in his sinus. On August 1, 2015, Dr. Weston Davis, DACVS, performed the surgical procedure on Blazer for an expansile paranasal sinus cyst of the left paranasal sinuses, extending to the right concho-frontal sinus.
Hopkins noticed that Blazer, who she calls “George” for his laid-back attitude, had a raised knot on his head this spring and consulted with her local vet, Dr. Kelly Alderman. The area was monitored closely and remained in a similar condition until June, when Hopkins noticed Blazer wheezing while running barrels and the knot increasing in size.
Diagnosing the Paranasal Sinus Cyst
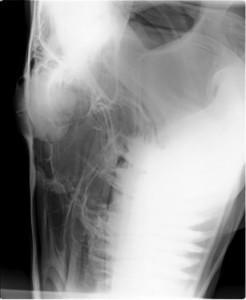
Dr. Alderman performed radiographs on the site and aspirated the swelling where a substantial amount of fluid was removed. She confirmed that the bump was a suspected paranasal sinus cyst. At that point, Blazer was referred to Dr. Weston Davis of Palm Beach Equine Clinic, who advised Hopkins that the cyst was likely growing slowly within the sinus for a considerable amount of time with no clinical signs. The diagnosis was an expansile paranasal sinus cyst of the left paranasal sinuses, extending to the right frontal sinus.
Paranasal Sinus Cyst Surgery
For surgery, Blazer was placed under standing sedation and local analgesia (painkiller) and his head was aseptically prepared before Dr. Davis performed a frontonasal sinusotomy (incision into the sinus). He made an opening from the middle of Blazer’s head to the corner of his eye. Once the skin flap was elevated and the bone fractured, a large amount of fluid was evacuated, which is consistent with the contents of a paranasal sinus cyst. Dr. Davis also observed that the sinus cavity was extremely distorted and expanded. The cyst lining was debrided and removed, then the sinus was lavaged and a tube was advanced into the sinus cavity to facilitate drainage. The sinus was packed with gauze tied together and soaked in a dilute betadine. Finally, the bone flap was replaced and the skin was closed and covered with a sterile bandage.
Recovery
The gauze packing was removed 48 hours after surgery and upon release from Palm Beach Equine Clinic, Hopkins was instructed to monitor the incision for heat, swelling and discharge. Bute, in the amount of 2g, was administered orally once a day for five days and Dr. Alderman removed the sutures after 10 days.
Hopkins characterizes Blazer as a sweet gelding with heart to spare, and is happy to report that his recovery has been fantastic. After six weeks of stall rest and rehab time to get back in shape, Blazer recently won his first barrel race after surgery. According to Hopkins, Blazer is running better than ever thanks to Dr. Davis and the staff at Palm Beach Equine Clinic.

